Traditional beta-blockers: what they do and what to watch for
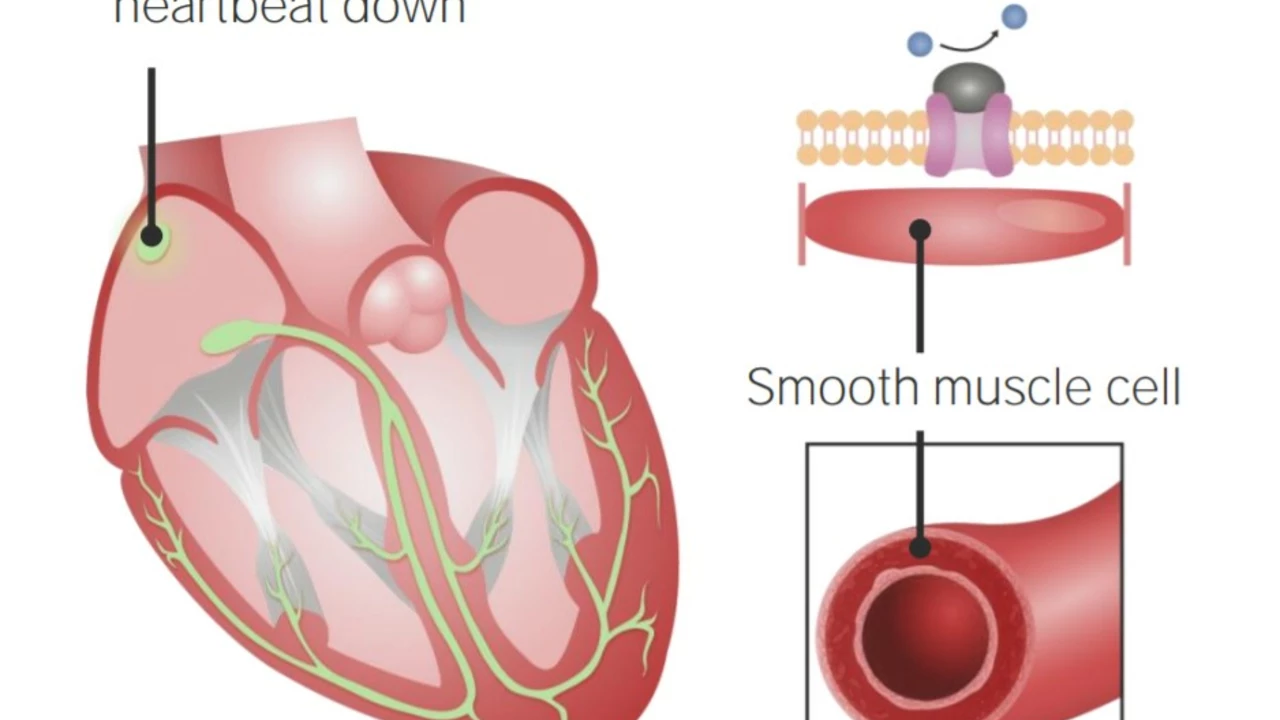
If you’ve been prescribed a beta-blocker or are curious about them, this short guide gives clear, practical info. Traditional beta-blockers like propranolol, metoprolol, and atenolol are older, well-studied drugs used for high blood pressure, certain heart rhythms, angina, migraine prevention, and sometimes anxiety or tremors. They slow the heart and lower blood pressure by blocking adrenaline’s effect on the heart.
Who benefits and who should avoid them
People with high blood pressure, heart failure (specific types), post-heart attack care, or recurring migraines often benefit. But not everyone should take them. If you have asthma or severe COPD, a traditional beta-blocker can tighten airways and cause trouble breathing. Diabetics need caution because beta-blockers can mask signs of low blood sugar like rapid heartbeat. Slow heart rate (bradycardia), certain heart block types, and some circulation problems are other reasons a doctor may avoid them.
Pregnancy and breastfeeding need special review—your doctor will recommend safe alternatives when needed. Don’t stop beta-blockers suddenly; sudden withdrawal can raise heart rate and blood pressure and even trigger chest pain.
Common side effects and simple checks
Most people tolerate these meds, but expect some side effects at first. Tiredness, cold hands and feet, mild dizziness, and slower pulse are common. Some people notice sleep changes or less sexual drive. Serious side effects like fainting, extreme shortness of breath, or very slow heartbeat mean call your clinician right away.
Simple things you or your doctor should check: measure resting heart rate and blood pressure before and after starting the drug, review current medicines for interactions, and track symptoms for the first few weeks. If you’re on insulin or sulfonylureas for diabetes, watch blood sugar more closely for the first month and learn non-heart-related signs of low sugar (sweating, confusion).
Interactions matter. Combining beta-blockers with calcium channel blockers (like verapamil or diltiazem) can slow the heart too much. Some antidepressants and certain over-the-counter cough meds can also change how the beta-blocker works. Tell your doctor about all prescription meds, supplements, and herbals.
Practical tips: start at the dose your provider suggests and follow up in 1–3 weeks if possible. If side effects are a problem, many people switch to a different beta-blocker or another class like an ACE inhibitor or ARB. If you plan surgery, tell the anesthesiologist about beta-blocker use—stopping right before surgery can be risky, so doctors often continue them.
If you want more detail on specific drugs or alternatives, check our related articles on blood pressure meds and treatment options. And always talk with your healthcare provider before changing doses or stopping a medication.