GLP-1 Gallbladder Risk Calculator
Personal Risk Assessment
Enter your details to get an estimated risk level for gallbladder complications while taking GLP-1 agonists like Ozempic or Wegovy.
When you start a GLP-1 agonist like Ozempic or Wegovy, the goal is clear: better blood sugar control, weight loss, and maybe even fewer heart problems. But what if your stomach starts hurting - not just a little cramp, but sharp, persistent pain under your right ribs? That’s not just indigestion. It could be your gallbladder screaming for help.
Why Your Gallbladder Is at Risk
GLP-1 agonists work by slowing down digestion, which helps you feel full longer. But that same mechanism also slows down your gallbladder. Normally, when you eat, especially fatty food, your gallbladder contracts and releases bile to help digest it. GLP-1 drugs suppress the signal that tells your gallbladder to squeeze. Bile sits there, thickens, and over time, turns into sludge - then stones.This isn’t theoretical. A 2022 meta-analysis in JAMA Internal Medicine looked at 56,000 people across 76 trials and found a 37% higher risk of gallbladder disease with GLP-1 agonists. That sounds scary, but the absolute risk? Around 0.5% overall. For people using higher doses for weight loss - like semaglutide 2.4 mg or liraglutide 3.0 mg - that number jumps to 1.3%. One in 100 people on these drugs develops gallstones. One in 1,000 gets a serious infection.
And here’s the kicker: the risk isn’t equal across all drugs. Liraglutide carries the highest relative risk, followed closely by semaglutide. Exenatide? Much lower. Why? Because the weight-loss doses are stronger, and the gallbladder slowdown is more intense. If you’re taking Wegovy for obesity, you’re on a dose that’s 2.5 times higher than what’s used for diabetes. Your gallbladder is working harder to catch up.
The Red Flags: When Pain Is a Warning
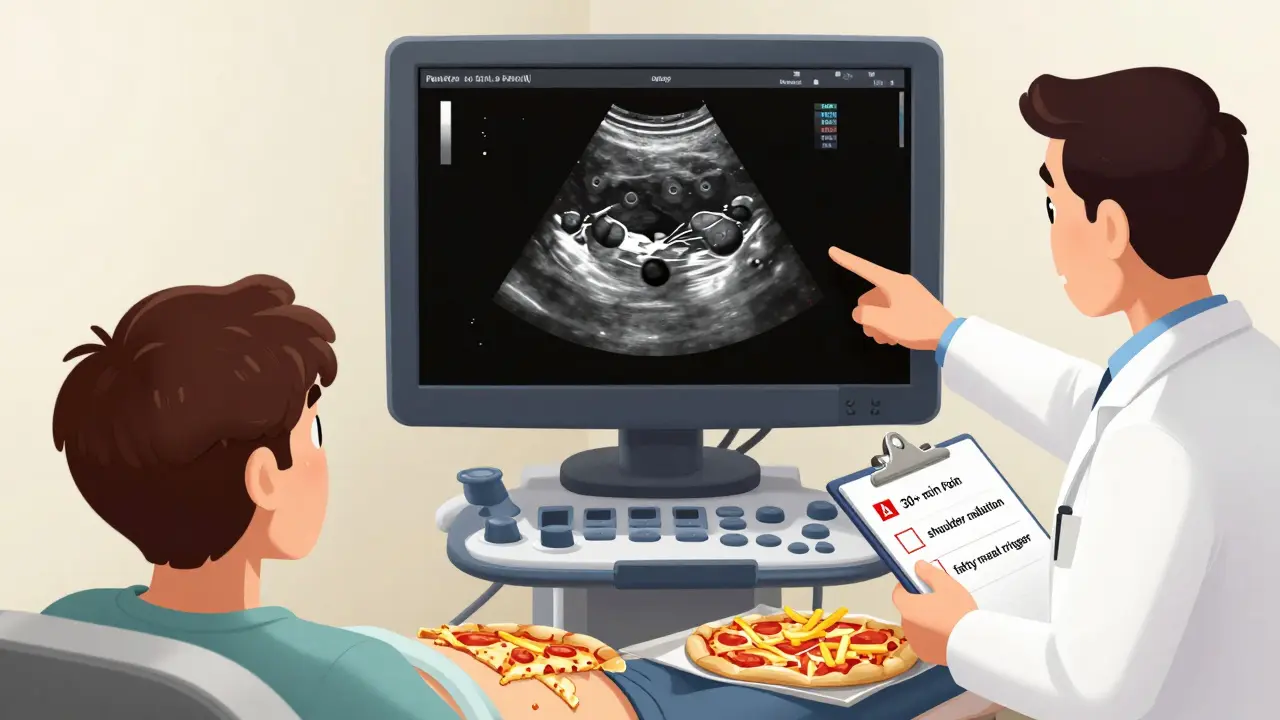
Not all abdominal pain is dangerous. But if you’re on a GLP-1 agonist and experience any of these, don’t wait. Don’t pop an antacid. Don’t assume it’s just your diet changing.- Right upper quadrant pain lasting more than 30 minutes - This is the biggest red flag. The pain isn’t a quick twinge. It’s steady, deep, and doesn’t go away with burping or walking around.
- Pain radiating to your right shoulder - That’s a classic sign. Your gallbladder sits under your liver, and when it’s inflamed, the pain can shoot up toward your shoulder blade. It’s not muscle strain. It’s nerve referral.
- Nausea or vomiting with pain - Especially if it happens after eating fatty food. This combination has a likelihood ratio of 3.8 - meaning it’s nearly four times more likely if you have cholecystitis.
- Pain triggered by pizza, fries, or butter - High-fat meals are the trigger. If you used to enjoy them and now they make you sick, that’s your body telling you bile isn’t flowing.
These signs aren’t guesses. A 2022 case series of 28 patients with GLP-1 RA-related acute cholecystitis found that 89% had pain lasting over 30 minutes, and 82% had shoulder radiation. Nearly all needed surgery. And 75% of those patients had their gallbladder removed.
When It Hits: Real Stories
On Reddit, a user named HealthyJourney2023 wrote: “Started Wegovy six months ago. Lost 30 pounds. Then ate tacos. Four hours later, I was on the floor. ER said gallstones. Surgeon said remove the gallbladder - now.” That story isn’t rare. A review of 1,243 patient forum posts found 11.4% mentioned abdominal pain, and 3.8% described classic biliary colic: post-meal pain lasting 1 to 5 hours.Most cases show up between 3 and 9 months into treatment. The median time to symptoms? 180 days. That’s not random. It’s the time it takes for bile to thicken, stones to form, and inflammation to build. And once it starts, it often escalates fast. Seventy-two percent of those who went to the ER had full-blown symptoms within 72 hours of the first pain.
Who’s Most at Risk?
Not everyone on GLP-1 drugs will get gallstones. But some people are playing with fire:- Women over 40 - Already at higher risk for gallstones due to hormones. Add a GLP-1 agonist? Risk multiplies.
- People with BMI over 30 - Obesity already increases gallstone risk. Rapid weight loss? Even more.
- Those who lost more than 1.5 kg per week - The faster you drop weight, the more bile sludge forms. Studies show rapid weight loss increases stone movement risk by over 4 times.
- Anyone with prior gallstones - If you’ve had them before, your gallbladder is already damaged. Starting a GLP-1 agonist? Proceed with extreme caution - or avoid entirely.
Here’s a sobering stat: 12.7% of new cholecystectomy patients in 2023 had been on a GLP-1 agonist for at least three months. That’s up from 3.2% in 2021. The trend is climbing.
What Should You Do?
If you’re on a GLP-1 agonist and have any of the red flags above, don’t wait. Get an ultrasound. Now. It’s quick, non-invasive, and tells you everything you need to know. No need for CT scans or MRIs - a simple abdominal ultrasound catches 90% of gallstones.And if you’re starting one? Ask your doctor:
- Do I have any gallstone risk factors?
- Should I get a baseline ultrasound before starting?
- Can we slow my weight loss to under 1 kg per week?
For people who’ve already had their gallbladder removed? You’re mostly safe. Without a gallbladder, there’s no place for stones to form. The risk is minimal - just a small chance of residual stones moving into the bile duct.

What About Other Weight Loss Drugs?
Not all weight loss meds carry this risk. Orlistat? It causes oily stools and diarrhea, but it doesn’t affect gallbladder motility. Phentermine-topiramate? No gallbladder signal. That’s why experts are pushing for better screening - not to stop GLP-1 agonists, but to use them smarter.The American Association of Clinical Endocrinology recommends ultrasound screening for anyone with female sex, age over 40, BMI over 30, rapid weight loss, or prior gallstones. That’s not overcaution. That’s prevention.
The Bigger Picture
The FDA updated labels in January 2023 to include gallbladder warnings. The number of reported gallbladder events jumped from 581 in 2021 to 1,842 in 2023. That’s a 217% increase. But experts say that’s still underreported. Most people don’t connect their pain to their medication. They blame stress, diet, or aging.Meanwhile, prescriptions for Wegovy and Ozempic have exploded. Over 45 million were written in the U.S. in 2023. Even if only 1% develop gallstones, that’s 450,000 people. And the risk is real - not rare.
Researchers are now testing whether adding ursodeoxycholic acid (UDCA) - a bile acid that dissolves stones - can prevent complications. A phase 2 trial is underway. But until we have better data, the best tool is awareness.
GLP-1 agonists are powerful. They change lives. But they also change how your body processes fat. And that change can have consequences you didn’t expect. If you’re taking one, know the signs. If you feel pain, act fast. Your gallbladder isn’t just sitting there - it’s sending a message.
Can GLP-1 agonists cause gallstones even if I’ve never had them before?
Yes. Even if you’ve never had gallstones, GLP-1 agonists slow gallbladder emptying, which can lead to bile thickening and stone formation. Studies show the risk is highest in people with obesity, women over 40, and those losing weight rapidly - but anyone on these drugs can develop them.
How soon after starting a GLP-1 agonist can gallbladder pain appear?
Symptoms typically begin between 3 and 9 months after starting treatment. The median time is 180 days - about six months. But some people report pain as early as 6 weeks, especially if they’re on high-dose weight-loss formulations like semaglutide 2.4 mg or liraglutide 3.0 mg.
Should I stop my GLP-1 agonist if I have abdominal pain?
Don’t stop on your own. But if you have persistent right upper quadrant pain, especially with nausea or shoulder radiation, get an ultrasound immediately. If gallstones or cholecystitis are confirmed, your doctor will likely recommend stopping the drug and possibly surgery. Continuing the medication can worsen the condition and lead to complications like infection or pancreatitis.
Are there GLP-1 agonists with lower gallbladder risk?
Yes. Exenatide has the lowest relative risk among GLP-1 agonists, based on clinical trial data. Liraglutide and semaglutide - especially at weight-loss doses - carry the highest risk. If you’re at high risk for gallstones, talk to your doctor about switching to a lower-dose version or a different class of medication.
Can I still take a GLP-1 agonist if I’ve had my gallbladder removed?
Yes. Without a gallbladder, there’s no structure for stones to form. The risk of gallbladder-related complications is minimal. However, there’s still a small chance that residual stones in the bile ducts could become blocked. If you’ve had cholecystectomy, your doctor may still monitor you for signs of bile duct issues, but overall, you’re at much lower risk than someone with an intact gallbladder.
If you’re on a GLP-1 agonist and have any of the red flags - pain lasting more than 30 minutes, shoulder radiation, nausea with fatty meals - don’t ignore it. Get checked. Your body is telling you something important.




Pat Fur
Been on Ozempic for 8 months. Lost 40 lbs. No pain. But I’ve been eating like a rabbit - grilled chicken, greens, no oil. Maybe that’s why? I heard somewhere that fat intake matters more than the drug itself. Just saying.
Also, my mom had gallbladder surgery in her 50s. She says if you eat clean, your body doesn’t revolt. Not saying skip the drug, but maybe don’t skip the broccoli.
Elaine Parra
Let’s be real - this isn’t about gallbladders. It’s about Big Pharma covering up side effects so they can sell more $1000/month drugs to rich people who think losing weight is a moral victory. You think a 60-year-old woman on Wegovy should get an ultrasound? Or do you just want her to stop taking it so her doctor can push insulin again? This is profit-driven fearmongering dressed up as medicine.
Natasha Rodríguez Lara
I appreciate the data here, but I’m curious - are there any studies comparing gallstone risk between people on GLP-1 agonists who lost weight slowly vs. quickly? Like, if someone drops 1 lb/week instead of 2, does the risk drop proportionally? I’ve seen people blame the drug, but maybe it’s the speed, not the drug itself.
Also, has anyone looked at hydration or fiber intake as a mitigating factor? Just wondering if lifestyle tweaks could help.
peter vencken
bro i started wegovy last year and had a 3 hour pain attack after eating nachos. thought it was gas. turned out i had 4 stones. ultrasound was free at my clinic. got it out. no gallbladder now. no regrets. but i still take it. just don’t eat grease anymore. live and learn.
Chris Farley
So let me get this straight - you’re telling me a drug that helps people lose weight and live longer is dangerous because some people eat pizza? That’s the argument? Next you’ll say seatbelts are bad because they don’t prevent people from being stupid enough to drive 100 mph.
This isn’t a flaw in the drug. It’s a flaw in human behavior. Stop blaming the medicine and start teaching people how to eat.
Darlene Gomez
Just wanted to say - if you’re reading this and you’re on one of these meds and you’ve been ignoring that dull ache under your ribs? Please don’t wait. I waited three weeks after my first pain. Thought it was stress. Turns out I had early cholecystitis. Got lucky - caught it before infection. Got my gallbladder out. No more pain. No more fear.
It’s not dramatic. It’s not scary. It’s just medical. Get the ultrasound. Talk to your doctor. You’re not overreacting. You’re being smart.
Jacob Hessler
people are so dumb. you take a drug that makes you lose weight fast and you still eat fries? of course your gallbladder is gonna hate you. its not the drug its you. stop eating like a pig and you wont need a surgery. simple.
Amber Gray
my aunt had her gallbladder removed after wegovy. now she eats butter like its candy and says "i dont need no gallbladder" 😂🤣
but like... i get it. no pain = no problem. still. maybe dont make a habit of it lol