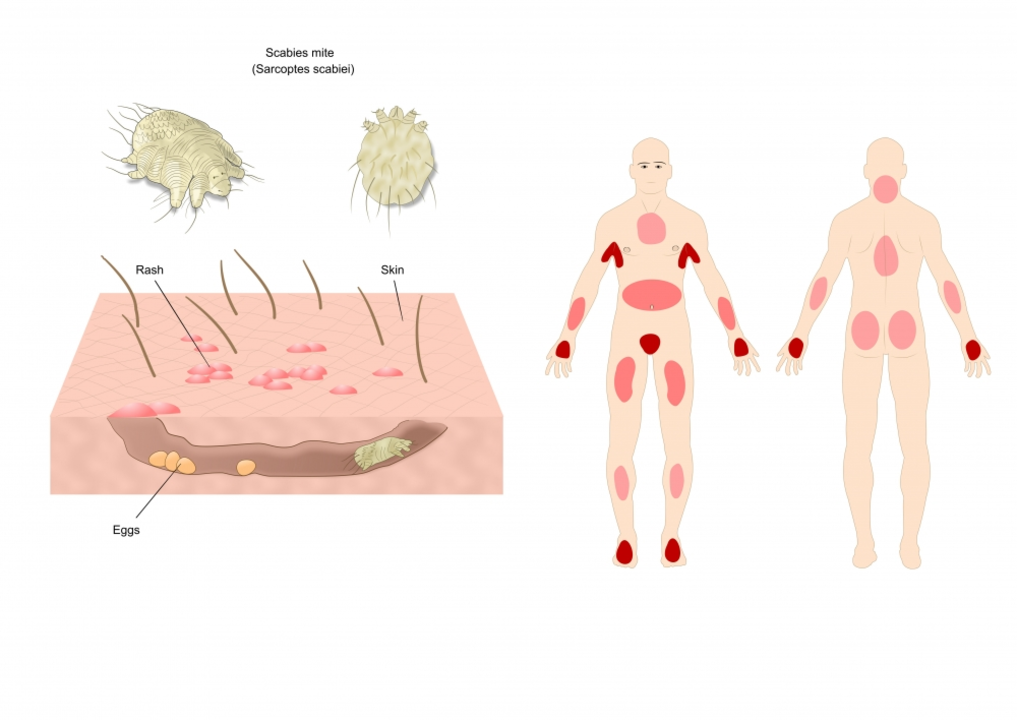
Sarcoptes scabiei: How to Spot, Treat, and Stop Scabies
Hit with intense itching at night? That could be scabies, caused by the tiny mite sarcoptes scabiei. These mites burrow into skin, lay eggs, and cause itchy rashes. They spread easily through close contact, shared bedding, or clothes. This page gives clear, practical steps: how to recognize it, what treatment works, and how to clean your home to avoid getting reinfected.
Symptoms are usually intense itching, small red bumps, and thin squiggly lines where mites burrow. Common spots are between fingers, wrists, armpits, waistline, and groin. Babies and elderly can get scabies on the head and face. If you or someone close has these signs, treat everyone in the household at once — even people without symptoms — because mites can hide for weeks.
Simple, effective treatments
First-line treatment is a prescription topical cream like 5% permethrin applied from neck to toes and left on for the time the doctor says (usually overnight). Oral ivermectin is another option, especially for widespread or crusted scabies, or when topicals fail. Follow your prescriber's directions exactly: repeat doses are often needed after a week. Over-the-counter anti-itch creams and antihistamines can ease symptoms while mites die off, but they don't cure scabies.
Crusted (Norwegian) scabies is a severe form with thick crusts and thousands of mites. It needs urgent doctor care and a stronger, often combined, treatment plan. If you see heavy crusting, rapidly spreading rash, or poor response to standard treatment, seek medical attention fast.
Cleaning and prevention that actually work
Wash bedding, clothing, and towels used in the last 3 days in hot water and dry on high heat. Items that can’t be washed should go in sealed plastic bags for at least 72 hours; mites die without human skin within 2–3 days. Vacuum furniture and carpets, and clean surfaces where skin may have shed. You don’t need to fumigate the house or use harsh chemicals — focus on laundry and vacuuming.
Avoid close skin-to-skin contact with anyone infected until they’ve completed treatment. For sexual partners, household members, and close caregivers, check with a clinician about preventive treatment. If symptoms persist after treatment, don’t assume failure — see a doctor. Reinfection can happen if a household member was missed, treatment wasn’t applied correctly, or items weren’t cleaned.
If you have a weakened immune system, eczema, or live in a care facility, scabies can be harder to treat and spread fast. Tell your provider about other health issues, medicines, or pregnancy before starting treatment. Don’t substitute home remedies for prescription therapy — they delay cure and risk complications. Follow up after treatment if itch or rash lasts beyond four weeks; post-scabetic itch can persist but needs different handling than active infection. Seek medical advice.
One last tip: document treatment and laundry steps so everyone follows the same plan. Scabies is unpleasant but curable. With the right medicine, good cleaning, and treating close contacts, you can stop sarcoptes scabiei and get back to normal fast.