Central pain syndrome: what it is and what helps
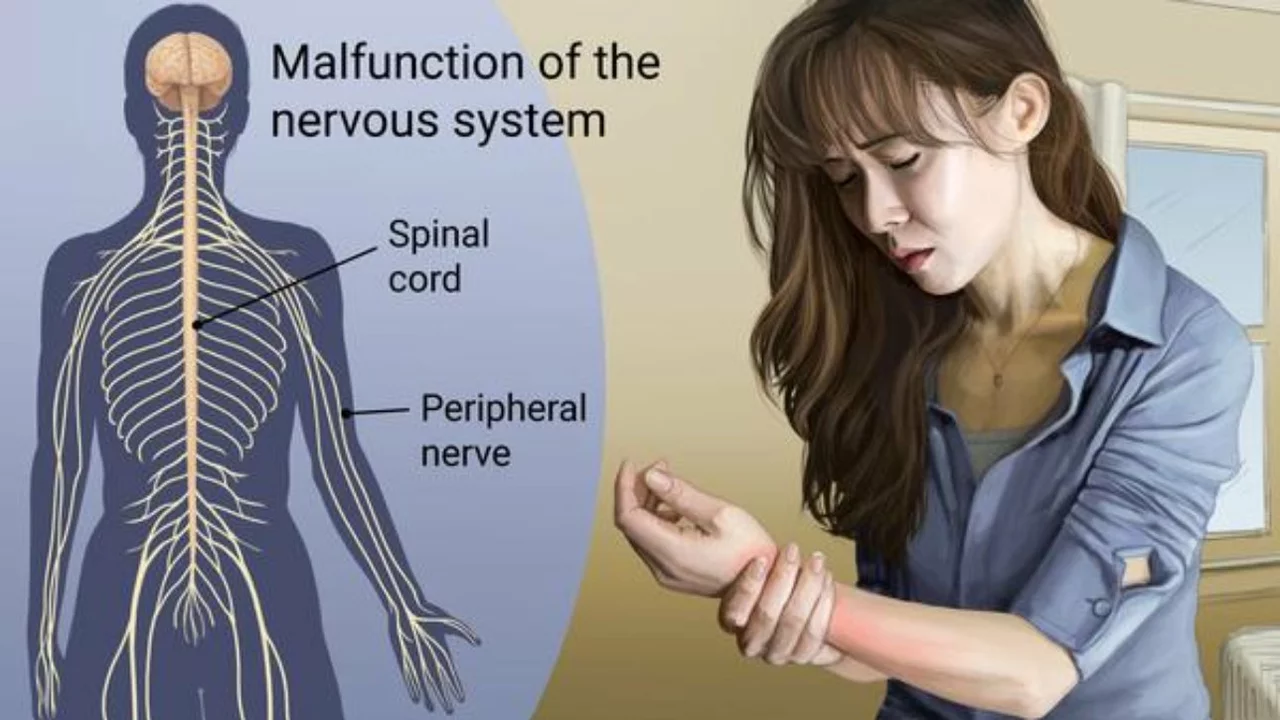
Central pain syndrome (CPS) is chronic pain that starts after damage to the brain or spinal cord. If you’ve had a stroke, spinal cord injury, multiple sclerosis, or severe head trauma and now feel burning, stabbing, or oddly electric pain, CPS could be the reason. This pain comes from damaged central nervous system pathways, so it behaves differently than ordinary muscle or joint pain.
What causes the pain and how it feels
Damage to sensory pathways in the brain or spinal cord scrambles how your nervous system reads normal sensations. A light touch can feel painful (allodynia) or a small poke can feel like a shock. Many people describe deep burning, pins-and-needles, or constant aching. Symptoms often start weeks to months after the injury and can fluctuate with temperature, stress, or activity.
Common triggers include stroke (post-stroke central pain), spinal cord injury, multiple sclerosis lesions, and traumatic brain injury. The exact pattern depends on where the damage sits — a small lesion in the thalamus can create widespread pain, while spinal cord injury tends to cause pain below the injury level.
Practical treatment steps that actually help
There’s no single cure, but you can reduce pain and improve function with a mix of treatments. Medications often tried first include anticonvulsants like gabapentin or pregabalin, certain antidepressants such as amitriptyline or duloxetine, and sometimes lamotrigine for post-stroke central pain. These medicines aim to calm overactive nerves. They don’t erase the cause, but many people get meaningful relief.
Non-drug options matter. Physical therapy that focuses on graded movement and retraining the nervous system can lower sensitivity. Cognitive behavioral therapy (CBT) helps with coping and sleep, which in turn reduces pain. Transcutaneous electrical nerve stimulation (TENS) can give temporary relief for some people. For severe, resistant cases, advanced options like spinal cord stimulation or targeted neuromodulation may be discussed with a pain specialist.
Be cautious with opioid medications: they often don’t work well for central neuropathic pain and carry risks. Instead, aim for a plan that mixes meds, rehab, sleep and stress management, and patient education.
Simple daily steps help more than you might expect. Keep a pain diary to spot patterns and triggers. Prioritize regular sleep, small exercise sessions you can sustain, and gentle temperature control if cold or heat worsens your pain. Small changes—cutting back on caffeine, using relaxation apps, or pacing activity—can lower flares.
See a neurologist or pain specialist if symptoms limit daily life. They can rule out treatable causes, adjust medications, and recommend nerve-targeted therapies. If you already have a diagnosis like MS or a prior stroke, ask your team specifically about central pain—early recognition speeds access to the most helpful treatments.
If your pain feels odd, intense, or keeps getting worse, get help. Central pain syndrome is tough, but with the right mix of medical care, rehab, and self-management you can regain control and improve your day-to-day life.